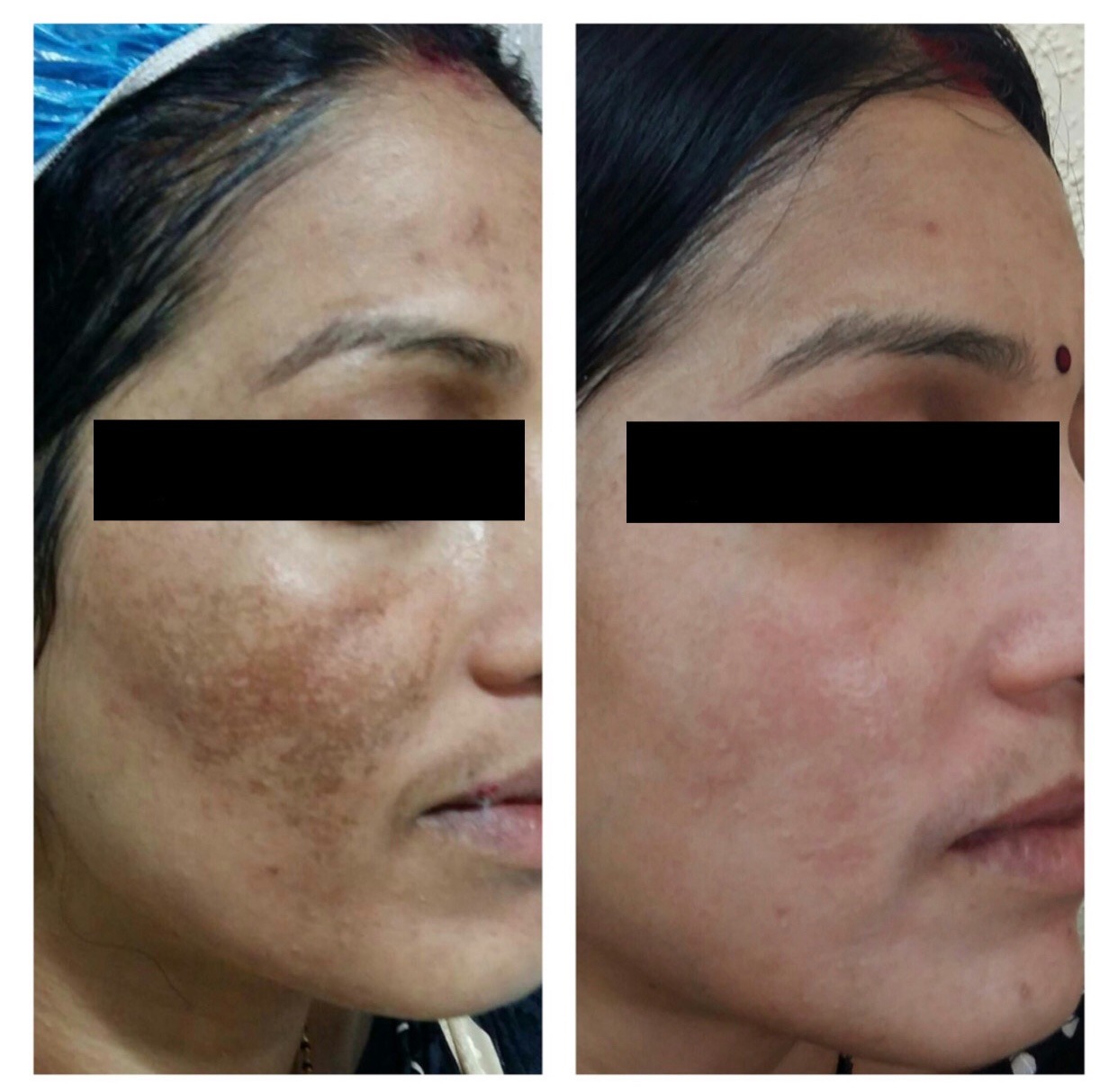
What Is Melasma?
Melasma, also known as chloasma, is a common skin condition characterised by skin discolouration, particularly dark patches of skin. Melasma is most commonly found in females, particularly when pregnant, in fact up to 50% of pregnant women experience symptoms, but men can also suffer from this condition. It is also commonly found in women taking hormonal contraceptive pills. Melasma is more common in those with darker skin tones and those who tan very quickly. Melasma is not contagious as it is not an infection so can’t be passed from one person to another, it is also not an indicator of skin cancer or of an allergy.
What Are The Symptoms Of Melasma?
Melasma can appear anywhere on the body which is exposed to the sun. It is most commonly seen on the face, particularly the cheeks, forehead, nose and chin, but is also found on the arms and neck. The areas of melasma will look darker than the surrounding skin and are flat to the skin not raised. Other than appearance, there are no physical symptoms of melasma. The affected skin is not painful or itchy but the condition may cause upset or embarrassment. Symptoms of melasma will become more notable in the summer months in response to sunlight.
What Causes Melasma?
The exact cause of melasma is not fully known. It is thought that the melanocytes in the skin, the pigment producing cells, produce too much pigment in certain areas.
Despite the fact that the cause is unknown, factors which may trigger melasma or make symptoms worsen have been identified. Changes in hormones can trigger melasma which is why it is so commonly seen during pregnancy. The contraceptive pill and other hormone replacements can therefore also be attributed. As with many skin conditions, exposure to UV light in the form of natural sunlight or sunbeds can trigger in people who have a family history of the condition.
How Is Melasma Diagnosed?
Melasma is relatively easy to diagnose and most experienced doctors and dermatologists will be able to diagnose this skin condition from looking at your skin. In rare cases, under local anaesthetic, a small section of skin may need to be removed and examined to eliminate any
How Is Melasma Treated?
There are a few ways in which melasma can be treated, both at home and in a medical setting. It is important to note that some of these treatments may not be suitable for those who are pregnant so it is important to discuss treatment options with a dermatologist in Indore.
Can Cause Skin Damage.
A consultation with a dermatologist will be required before any treatment takes place to
While skin problems aren’t prejudicial, melasma is an adamant, annoying one that’s chartered mostly for women, but men get victimized to the violent affliction too.
Flash Facts about Melasma:
- Melasma is also known as the mask of pregnancy or cholasma Melasma is common in women aged between 20 to 50 years old.
- An SPF of 30 gives 97% protection from the sun’s harmful rays and UV rays, while SPF 45 provides 98% protection. It’s currently impossible for any SPF to offer 100% protection from the sun, so don’t believe the ballyhoo!
Certain Characteristics of Melasma
Melasma forms in definite patterns which can be easily identified either as spots on the skin similar to freckles or brown patches of rough skin that grow bigger with time. Some of these patterns are:
- Malar pattern: This develops on the cheeks and nose
- Mandibular pattern: Begins forming around the jaw line
- Brachial melasma: This appears on the shoulders and the upper arms and shoulders
- Lateral cheek pattern: Grows symmetrically over the cheek on both sides of the face
- Centrofacial pattern: Forehead, cheeks, Nose, and Upper lips
Melasma can be brought on bys
- Sun exposure: One of the most common causes of the skin pigmentation problem amongst both males and females continues to be sun exposure. It may not only lead to Melasma pigmentation but incite sun damaged skin in form of blotchy patches, brown spots and dryness etc. Excessive exposure to sun is known to activate the melanocytes within the body which begins producing more melanin.
- Family History: More than 30% of patients whether, women or men (particularly in Japan) suffering from melasma have a family history of pigment disorder. The cogeital irregularity in dermal pigmental can be acquired by the mother, grandmother or sister who suffer from it. So, here again genes are guilty. Have a check on your family tree to see if others in your family have or have had this skin condition. Doing so would somewhat help with self-diagnosis or offer your.
- Pregnancy: Attributed as one of the primary cause of melasma, the chief trigger has often been credited to hormonal alterations that a woman goes through due pregnancy period, (mainly in the second or third trimester of pregnancy).
- Hormone replacement therapy: Receiving hormone replacement therapy also can have Melasma due to changes in hormonal balance during the treatment.
In addition to contraceptive pills, other drugs that can stimulate the skin to darken or promote skin’s sensitivity to the sun causing skin darkening are:
- Antipsychotics
- Antimalarials
- Amiodarone
- Cytotoxic drugs/chemotherapeutics
- Phenytoin
- NSAIDs (non-steroidal anti-inflammatory drugs)
- Tetracycline antibiotics (like minocycline, doxycycline etc.)
- Stress: Long span of stress on the body and mind can also encourage hormonal alterations, thuscausing Melasma.
- Thyroid problems: Anyone suffering from Hypothyroidism or low levels of the thyroid hormone can get a trigger to other hormonal changes which can further cause this skin disorder. With patient’s visit ratio, it has also been observed that people usually with darker skin tone tend to get melasma and it is less prevalent in people with fairer skin.
Types of Melasma
- Epidermal
- Dermal
- Mixed
Where is Melasma seen on the body?
Melasma is clinically depicted by discoloration or hyperpigmentation predominantly on the face. There are 3 types of common facial patterns that have been determined in melasma, including centrofacial (center of the face), mandibular (jawbone), malar (cheekbones).
Dermatologist Treatment Options
- AHT (Chemical Peeling)
- Lasers (Q-Switch Laser)
- Photo Facials
- Face PRP
- Mesotherapy
How common is melasma?
Melasma is a very common skin disorder, especially among pregnant women. 15% to 50% of pregnant women get it. Between 1.5% and 33% of the population may get melasma and it happens more often during a woman’s reproductive years, and rarely happens during puberty. It usually starts between 20 and 40 years of age.
Who is at risk of melasma?
More likely to get melasma than men: about 10% of those who get melasma are men, 90% women.
Your epidermis contains cells called melanocytes that store and produce a dark color (pigment) known as melanin. In response to light, heat, or ultraviolet radiation or by hormonal stimulation, the melanocytes produce more melanin, and that’s why your skin darkens.
Why do women get melasma when they’re pregnant?
Pregnant women have increased levels of the hormones estrogen and progesterone. These hormones are thought to contribute to your melasma.
Conditions commonly confused with melasma include:
- Atropic linchen.
- Drug-induced pigmentation.
- Pigmentary demarcated line
- Lentigo (age spots). Nevus of Hori.
- Nevus of Ota.
- Postinflammatory pigmentation.
Are freckles melasma?
Spots of melasma can sometimes be mistaken for freckles but they are not the same skin condition.
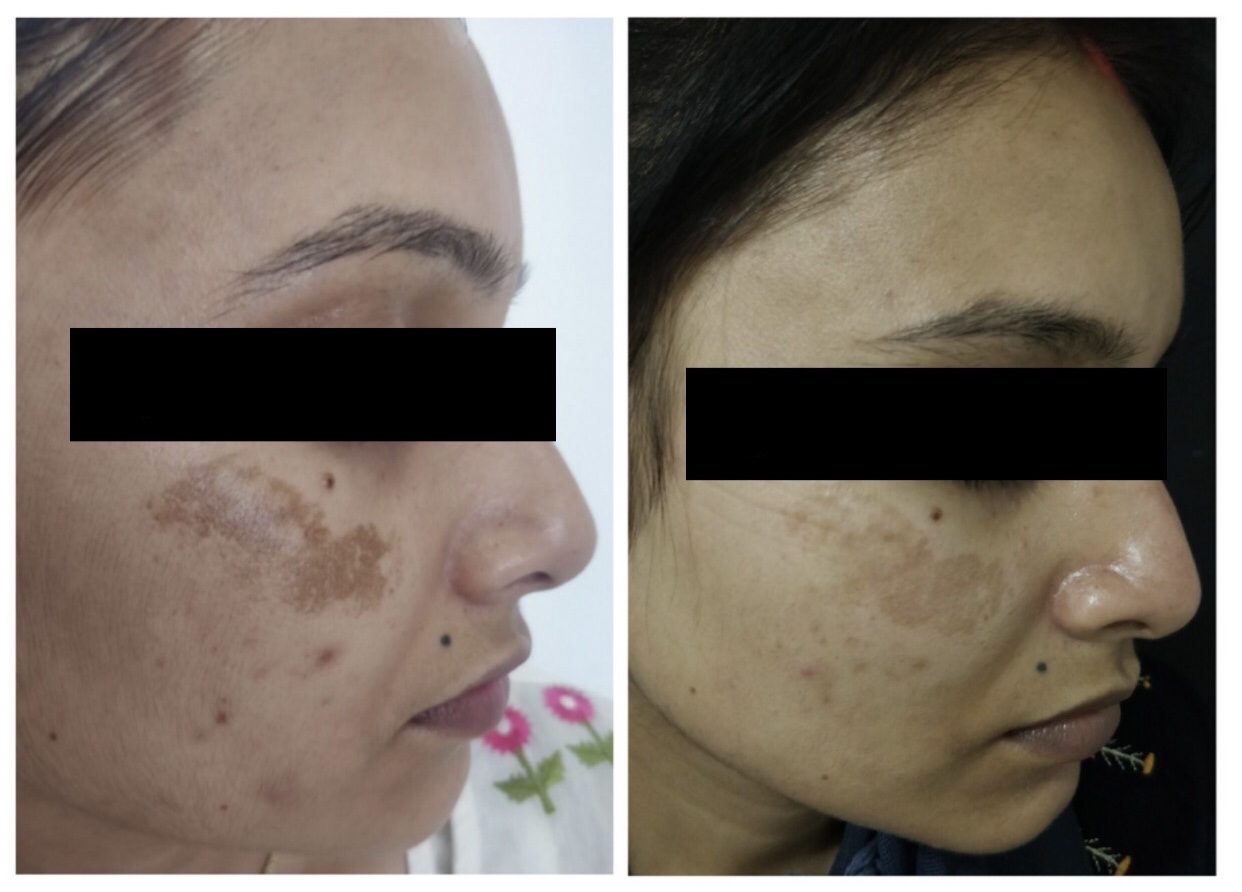
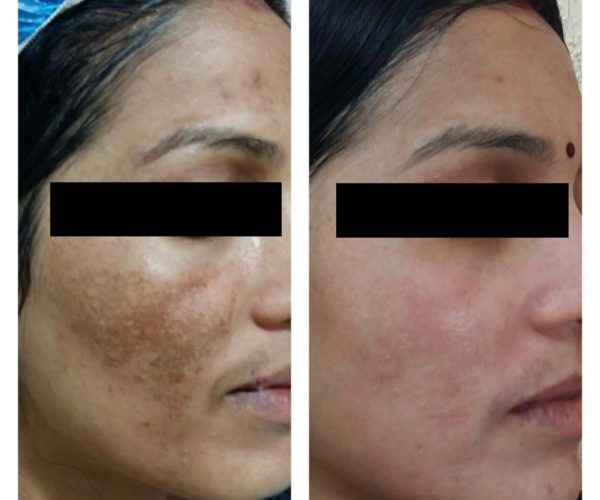
Results:


Equipment

